While the term is often used interchangeably with heart failure, congestive heart failure signifies a more severe form. It occurs when fluid backs up in the veins, leading to congestion.
What is Heart Failure?
Heart failure is a medical condition in which your heart isn’t pumping the necessary amount of blood your body needs. This failure may stem from the weakening of the heart muscle, resulting in reduced pumping capacity, or from the stiffening of the heart muscle, hindering its ability to relax and fill with blood, or both. In either case, the heart is unable to get enough blood to the body.
There are two types of heart failure:
CHRONIC
A gradual, long-term condition. This is the most common type and demands medical treatment and lifestyle adjustments to prevent life-threatening situations.
Acute
Which can onset suddenly.
Key Definitions
This measures the amount of blood the left ventricle pumps out with each contraction. A normal EF falls between 50% and 70%.
Occurs when the heart chambers stiffen, impeding sufficient blood filling.
Involves the enlargement of heart chambers over time, leading to inadequate blood pumping.
The left ventricle can’t pump enough blood to meet the body’s demands.
The right ventricle is too weak to supply sufficient blood to the lungs, causing vein congestion.
This occurs when both sides of the heart are affected by heart failure
Stages and Classes
As you familiarize yourself with the various types and severity levels of heart failure, you will come across terms like stages and classes. These measurements play a crucial role in diagnosing the disease’s severity and tailoring an appropriate treatment plan.
Stages of Heart Failure:

Classes (Functional Classes):
These classes measure an individual’s tolerance to physical activity on a scale from one to five.
Class I:
No extreme fatigue, irregular heartbeat, or breathing difficulties during ordinary activities.
Class II:
Comfortable at rest, but normal activity induces fatigue, irregular heartbeat, and breathing issues.
Class III:
Extreme symptoms arise during minor activity.
Class IV:
The heart struggles even at rest, causing discomfort with any activity.
CAUSES AND RISK FACTORS
The origins of heart failure are diverse, with various long-term or acute factors contributing to heart damage, such as heart attacks or persistent high blood pressure. Some of the most common include:

Additionally, heart failure can be caused or exacerbated by chronic conditions or traumatic events in the body such as:
SIGNS AND SYMPTOMS
While some people with heart failure may not have any symptoms or experience only mild ones, it is important to note that symptoms can fluctuate and vary among individuals. In many cases, symptoms tend to intensify gradually over time. Recognizing the signs of heart failure is crucial for timely intervention. Common symptoms include:

Treating and Managing Heart Failure
Upon diagnosis, your medical team will work with you to come up with a plan to manage your heart failure that can include a combination of medications, devices, surgery, and lifestyle adjustments. While heart failure isn’t curable, the treatment can be designed to slow its progression.

Depending on your specific diagnosis, your doctor may prescribe medications tailored to your needs. Common classes include beta blockers, ACE inhibitors, ARNIs, diuretics, and SGL2 inhibitors.
Some individuals with heart failure may require the assistance of devices. These devices serve various purposes, acting as a form of treatment, a bridge to heart transplant, or aiding in monitoring heart failure to minimize hospitalization. They can be either implanted in the body or external.
Abnormal heart rhythms, such as those that are too fast, too slow, irregular, or a combination, are common in some heart failure patients. Among the devices designed to restore normal heart rhythm are pacemakers, Cardiac Resynchronization Therapy (CRT), Implantable Cardioverter Defibrillators (ICDs) and Left Ventricular Assist Device (LVAD).
- Pacemakers: These devices are implanted if the heart beats too slow or too fast.
- Cardiac Resynchronization Therapy (CRT): When the symptoms of heart failure are severe, they may result from a lack of coordination between the bottom chambers of the heart (the ventricles), causing them to beat out of sync. In such cases, implanting a CRT device, called a ‘biventricular pacemaker’, can help synchronize the heart muscle contractions, thus improving its pumping function.
- Implantable Cardioverter Defibrillator (ICD): When the heart exhibits life-threatening irregular rhythms, an ICD may be attached to restore it to the proper rhythm. ICDs play a crucial role in preventing sudden cardiac death in patients experiencing ventricular fibrillation (fast and irregular heartbeats) and ventricular tachycardia (excessively rapid heartbeats in the lower chambers).
- Left Ventricular Assist Device (LVAD): In cases where the heart weakens significantly, a LVAD might be necessary. This mechanical pump can be employed while awaiting a heart transplant or as a standalone treatment for heart failure.
Advanced Monitoring Technologies – there are some new implantable devices designed to effectively manage your heart failure and minimize hospital visits. Innovative sensors can be strategically placed within the heart, offering real-time monitoring of heart pressure, fluid levels, and cardiac pumping efficiency. These advancements aim to enhance control over your heart failure condition, providing valuable insights for proactive care.
There may be situations where your doctor may recommend heart surgery or other procedures. These interventions can help with heart failure, but they are only performed when the benefits are more significant than the risks. Procedures intended to improve heart failure include coronary artery bypass, valve replacement or replacement, and heart transplantation.
Heart failure treatments are pivotal for maintaining your well-being. Not all treatments are universally applicable, so it is crucial to monitor your symptoms and communicate openly with your doctor about any changes. Never alter your treatment without consulting your doctor.
It is important to be fully present and active in your own treatment plan. While doctors have medical knowledge, you have vital and valuable knowledge too. You know yourself — your lifestyle, preferences, and priorities — better than anyone else. Here are a few ways to be an active participant in your own treatment plan:
- Preparing questions: Write down questions before appointments. Explore the questions provided further below that you can ask your doctor for further guidance.
- Seeking understanding: Continuously ask questions until you grasp the information.
- Having support: Bring a friend or family member to assist with taking notes and advocating on your behalf.
- Expressing preferences: Share your opinions, state your preferences, and communicate your needs to your care team.
Lifestyle – Living with Heart Failure
Lifestyle is a crucial factor in thriving with heart failure. Your doctor may recommend lifestyle adjustments, including avoiding alcohol and tobacco and making dietary changes. Embracing these changes step-by-step can make a significant difference. Here is some advice from heart failure patients themselves:

Follow your treatment plan exactly as you were told. Taking medications as instructed is vital for feeling better and enhancing your longevity. If you have any uncertainties, don’t hesitate to reach out to your doctor.

Heart failure symptoms vary among individuals. Find the symptom management tools that work best for you. Understanding and responding to changes in symptoms empower you to stay ahead of potential challenges.

Make the recommended dietary changes, such as reducing salt intake, managing liquids, and eliminating foods that may counteract your medications. Your diet plays a crucial role in supporting your overall health.

Physical activity makes a huge difference, even when it feels impossible. Becoming more active, even a little bit at a time, is good for the body and mind. Consult with your healthcare team to determine a suitable exercise routine.

Keep track of changes in symptoms, fluctuations in weight, or any other noticeable shifts in your body. Discuss your observations with your doctor to refine your management plan and address emerging concerns.

Boost your confidence in self-care by learning more about your heart disease. Use reliable sources to gather information and make informed decisions regarding your health. Knowledge is a powerful tool on your journey.

Maintain connections with supportive individuals in your life and seek out peers who share similar experiences. Building an emotional support network is crucial for staying motivated and focused on your health goals. Share your journey, seek advice, and offer support to others in your community.
Questions to Ask Your Doctor
As you embark on your journey of managing heart failure, engaging in open and insightful discussions with your healthcare provider is crucial. Here are some questions to consider, fostering a collaborative and informed approach to your heart health:
- Unravelling the origins: What caused my heart failure?
- Assessing severity and stage: How severe is my heart failure? What is the stage and level of my heart failure?
- Understanding ejection fraction: What is my ejection fraction?
- Foreseeing consequences: What might happen if I don’t do anything about my heart failure?
- Tailoring lifestyle adjustments: What changes should I make to my diet and exercise routines?
- Exploring medication options: Are there medications I can take to help me feel better?
- Navigating treatment choices: What treatment options are available for me, and what are the risks and benefits of each option?
- Monitoring heart health: How can I monitor my heart failure? Can I monitor at home?
- Recognizing signs and seeking guidance: What specific signs or symptoms should prompt me to contact my doctor?
Make a list of any additional questions that come to mind and ensure they are addressed by your healthcare provider, taking the time to fully understand the answers.
Additional Resources

Check Your Heart Failure Risk if You Have Diabetes
A clear, practical leaflet designed to help people living with diabetes understand their risk of heart failure, the importance of early testing, and the steps they can take to protect their heart health.

Understanding Heart Failure Discussion Guide – English Northern Ireland
A helpful discussion guide designed to support conversations between patients, carers, and healthcare teams about diagnosis, treatment, and management of heart failure.

Living with Heart Failure Whiteboard Animation – English Northern Ireland
A short, easy-to-understand animated video explaining heart failure, its impact on daily life, and how treatment and support can make a difference.

Heart Failure GoToGuide – English Northern Ireland
A detailed patient and caregiver guide explaining what heart failure is, its causes, symptoms, treatment options, and ways to live well with the condition.
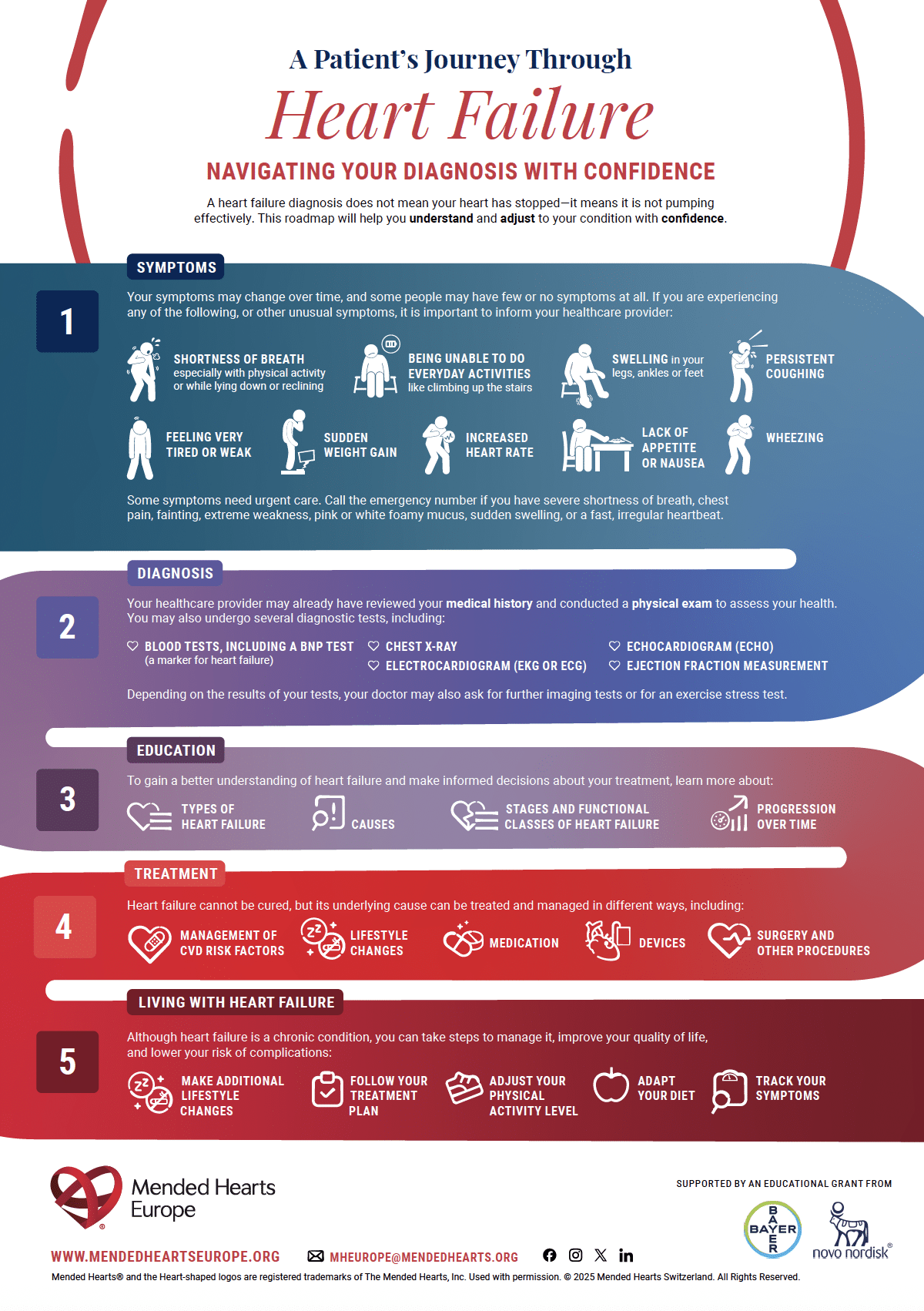
A Patient’s Journey Through Heart Failure – English Northern Ireland
An illustrated infographic following the patient journey from first symptoms through diagnosis, treatment, and long-term care for heart failure.

A Patient’s Journey Through Heart Failure
An illustrated infographic following the patient journey from first symptoms through diagnosis, treatment, and long-term care for heart failure.

























